Sutures
Suture materials
The purpose of a suture
Choice of a suture will depend on:
Natural suture materials
Synthetic suture materials
Absorbable suture are broken down by either:
Catgut
Silk
Vicryl
Polydioxone
Common errors of suture use
|
https://www.surgical-tutor.org.uk/default-home.htm?core/preop2/sutures.htm~right
SILK: animal protein, relatively inert for human tissue, loses
strength over long periods. Silk sutures are multifilament and provide a
potential haven for bacteria.
CATGUT: from the submucosa of the bovine intestine, eventually
resorb. It excites considerable inflammatory reaction and tends to potenciate
infections. It loses strength rapidly and it?s of little use in modern surgery.
SYNTHETIC NONABSORBABLE SUTURES: generally inert and retain strength
longer than wire. They must usually be knotted at least four times because of
their poor handling characteristics, resulting in retained foreign bodies.
SYNTHETIC ABSORBABLE SUTURES: strong, with predictable rates of loss
of tensile strength, incite a minimal inflammatory response and may have
special usefulness in gastrointestinal urologic and gynecological surgeries.
TAPES: skin closure of choice for clean or contaminated wounds, with
minimal probability of infections. They cannot be used in actively bleeding or
complex surface wounds.
Chronic Wounds
The first principle in managing chronic wounds is to diagnose and treat any
underlying circulatory disease. The second principle is never to allow open
wounds to dry. A third principle, but not less important, is to control any
infections with adequate care of the lesion and systemic antibiotics. Finally,
its also necessary to recognize that chronically scarred tissue is usually poor
perfused. Debridement of unhealthy tissue, often followed by skin grafting, may
be required for healing.
Wound Healing and Repair
Just after a surgical incision, a number of epithelial cells and connective
tissue cells die and the basement membrane is disrupted. This clean and
uninfected injury is enough to target an inflammatory response that will be
absolutely necessary for the wound healing. Immediately after the incision, the
wounds covered with clotted blood containing fibrin and blood cells. This
fibrin clots receives within 24 hours an amount of neutrophils, attracted by
inflammatory factors locally released. At this time, we also have mitotic
activity of the basal layer of the epidermis. By the day 3, macrophages are the
most common cells in the tissue, instead of neutrophils. The main feature at
this moment is the granulation tissue, that consists of fibroblasts and new
capillary with amorphous substance all around. By the 5th day, granulation
tissue and neovascularization are maximal. Collagen fibrils are present and
begin to bridge the incision, following the epithelial migration. After 1 week
there is still connective tissue proliferation, but inflammatory features have
virtually disappeared. At the end of the first month, the scar is completed
within an intact epithelial layer, covering a new cellular connective tissue
net, devoid of inflammation.
In some instances, the wound (not surgical ones) has a large loss of cells
and tissues, which makes the normal healing event impossible. In this case, we
have the healing by second intention. This is characterized by a more
complicated process with much more inflammation and granulation tissue. The
original architecture is never attained and the main feature of the phenomemon
is called ?wound contraction?. The wound contraction is caused, at least in
part, by the presence of myofibroblasts ¾ altered fibroblasts that have
ultrastructural characteristics of smooth muscle cells.
As noted, the disposition of connective tissue matrix, specially collagen,
its remodeling into a scar and the acquisition of wound strength are the
ultimate effects of the repair.
The wound healing process is influenced by many systemic and local host
factors. Nutrition state of the patient is very important. Protein deficiency
and particularly ascorbic acid deficiency inhibits collagen synthesis and
impairs healing. Glucocorticoids therapy, by its anti-inflammatory aspects,
retards healing. Patient?s age is also an systemic factor that plays a role.
Local infections are important causes of complicating and delaying healing
process. Hemorrhagic factors, such as ischemia, play a role and foreign bodies,
such as sutures and/or other fragments constitute impediments to healing.
The healing process may occur abnormally. There are many aberrations of
growth, but the most common is called keloid. Keloid is a tumoral scar resulted
from accumulation os excessive amounts of collagen. The reasons for keloid
formation still remain unknown, but is known that it?s more common in
afro-caribbeans.
https://www.medstudents.com.br/cirur/cirur3.htm
Suture size is based on strength and diameter as decided by the United
States Pharmacopeia (U.S.P.) This system uses “0” as
the baseline, average size suture. As suture diameter decreases,
“0’s” are added or numbers followed by a “0” (for example,
000 and 3-0 are the same size). As suture diameter increases above
“0”, numbers are assigned to the suture material.
https://cal.vet.upenn.edu/surgery/5051.htm
https://www.favormed.com/e18.htm
|
Examples of Suture Sizes for Use in Animals |
||||
|
10-0 – 8-0 |
7-0 – 5-0 |
4-0 – 3-0 |
2-0 – 0 |
1 – 2 |
|
Microvascular |
Vein/arterty repair |
Skin & Subcutis |
Abdominal Fascia |
Rib Retention |
|
Increase or decrease abdominal fascia and retention sutures appropriately |
||||
https://www.vetmed.auburn.edu/~hendera/guide/sutsize1.htm
General
Un-coated braided sutures may provide increased resistance to passage
through the tissues and may harbour bacteria within the braid.
Braided sutures are however easier to use and knots tend to be more secure
Coating a braided suture gives the suture qualities more like a mono-filament
suture
Mono-filament sutures are generally easy to use with easy passage through
tissue but may not hold a knot well. They also usually result in low tissue
reactivity and the smooth surface does not harbour bacteria.
Natural materials generally result in greater tissue reactivity
https://www.orthoteers.co.uk/Nrujp~ij33lm/Orthsutures.htm
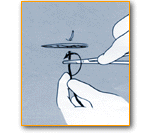
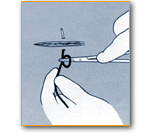

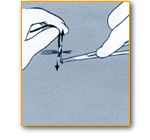

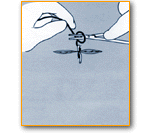
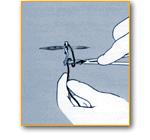
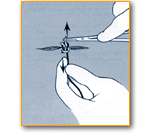
Suturing Tips
- In larger wounds muscle, membranes, fat and skin should be sutured separately.
- Subcutaneous sutures should be absorbable.
- Suturing goal should eliminate all pockets and dead space below skin; else allow drainage for fluid buildup.
- Suturing of fat reduces dead space.
- Use minimal tension on skin closures to prevent crushing injuries which delay healing.
- Cleansing of wound should only be done by lavage of sterile fluids. Never use caustic cleansing agents such as alcohol, hydrogen peroxide or other anti-bacterial agents; these will distrupt the natural inflammatory response and fibrin clot necessary for healing and potentially damage surrounding healthy tissue.





